Conditions We Treat
Comprehensive rheumatology care focused on relieving pain, reducing inflammation, stopping the progression of disease, and improving quality of life through personalized, evidence-based treatments.

Osteoarthritis (OA) is a common joint disease that affects middle-aged elderly people. This is commonly referred to as "wear and tear" arthritis, but OA is a disease of the entire joint, involving the cartilage, joint lining, ligaments, and bone.
What Are Common Treatments?
The goal of OA treatment is to reduce pain, improve function, and have a better quality of life.
Exercise can improve your muscle strength, decrease joint pain and stiffness, and lower the chance of disability due to OA. Weight loss can also help; for every 10 pounds of weight you lose over 10 years, you can reduce the chance of developing knee OA by up to 50 percent.
At our clinic we offer patient’s evaluation for possible drug therapies include oral pain relievers such as acetaminophen or nonsteroidal anti-inflammatory drugs (often called NSAIDs), which decrease swelling and pain.
Cymbalta is also sometimes prescribed to reduce pain, and patients with more serious pain may need stronger medications, such as prescription narcotics.
Joint injections with corticosteroids (sometimes called cortisone shots) or with a form of lubricant called hyaluronic acid can give months of pain relief from OA.
Surgical treatment becomes an option for severe cases and in this case the patient may be referred to orthopedic surgery for evaluation of deemed appropriate.
Osteoarthritis:
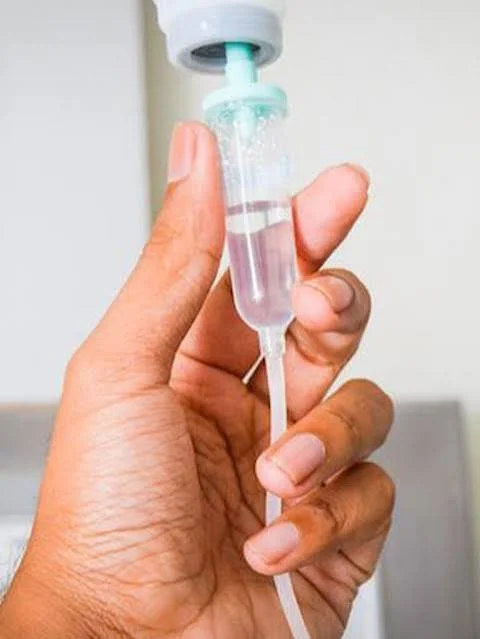
Biologic Therapy with Tumor Necrosis Factor (TNF) Inhibitors
TNF inhibitors are drugs commonly used in Rheumatology that help stop inflammation and are used to treat autoimmune inflammatory conditions such as rheumatoid arthritis, psoriatic arthritis, juvenile idiopathic arthritis, inflammatory bowel disease (Crohn’s and ulcerative colitis), ankylosing spondylitis and psoriasis, as well as others rheumatologic conditions.
The TNF inhibitors approved by the FDA are called infliximab, adalimumab, etanercept, golimumab, and certolizumab. These agents can be used by themselves or in combination with other medications such as prednisone, methotrexate, hydroxychloroquine, leflunomide or sulfasalazine.
How To Take It
TNF inhibitors can be administered in two ways. One way is by self-injection, with a very small needle that delivers the medication just underneath the skin of the thighs or the abdomen. These medications can be given weekly, every other week, or every 4 weeks. The second way is via an intravenous infusion every 4–8 weeks. This is done in healthcare facilities and can take a few hours.
Most patients feel better after 2 or 3 doses, but it may take 3 months to see the full benefit.
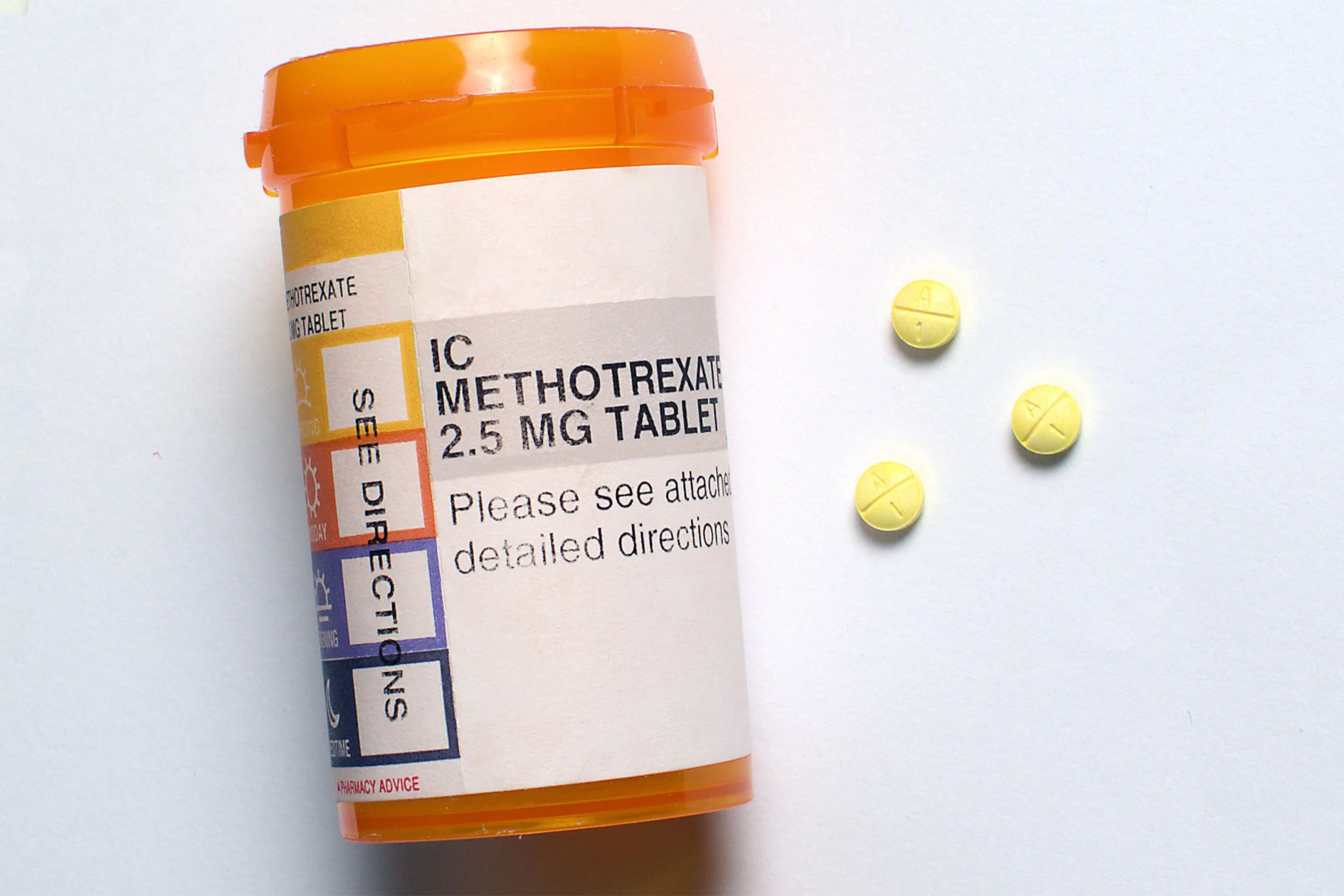
Methotrexate in the form of oral weekly pills or subcutaneous injections is one of the commonly used medications in the treatment of rheumatoid arthritis (RA). It may also be used to treat inflammatory myositis, vasculitis, psoriasis, psoriatic arthritis, scleroderma, and some forms of juvenile arthritis.
It is known as a disease-modifying anti-rheumatic drug (DMARD), because it not only decreases the pain and swelling of arthritis, but it also can prevent damage to joints, slow down the progression of disease, may prevent permanent joint damage and long-term disability.
How To Take It
Methotrexate comes as once week pills or as a subcutaneous injection. Methotrexate is usually taken as a single dose once per week, although occasionally the dose is split into two to improve absorption or avoid side effects. It is prescribed with vitamin folic acid (or folate) supplement to decrease the chance of side effects. Alcohol should be avoided as it can significantly increase the risk for liver damage while taking methotrexate. For childbearing women, two methods of contraception are recommended while using methotrexate, as it may cause severe fetal abnormalities and considered teratogenic.
Regular laboratory monitoring is required while taking methotrexate every 3-6 months.
Symptomatic improvement can be noted within three to six weeks of initiating therapy, but the full benefit of this drug may take up to 12 weeks.
Dr. Lopez (or My) personal advise is to start therapy on a day you can rest to let your body properly adjust to the new treatment and rest if necessary.
Always tell your trusted Rheumatologist if any new symptoms arise or any questions on your follow up appointment regarding your therapy. We are happy to answer any questions and clarify any concerns.
Methotrexate
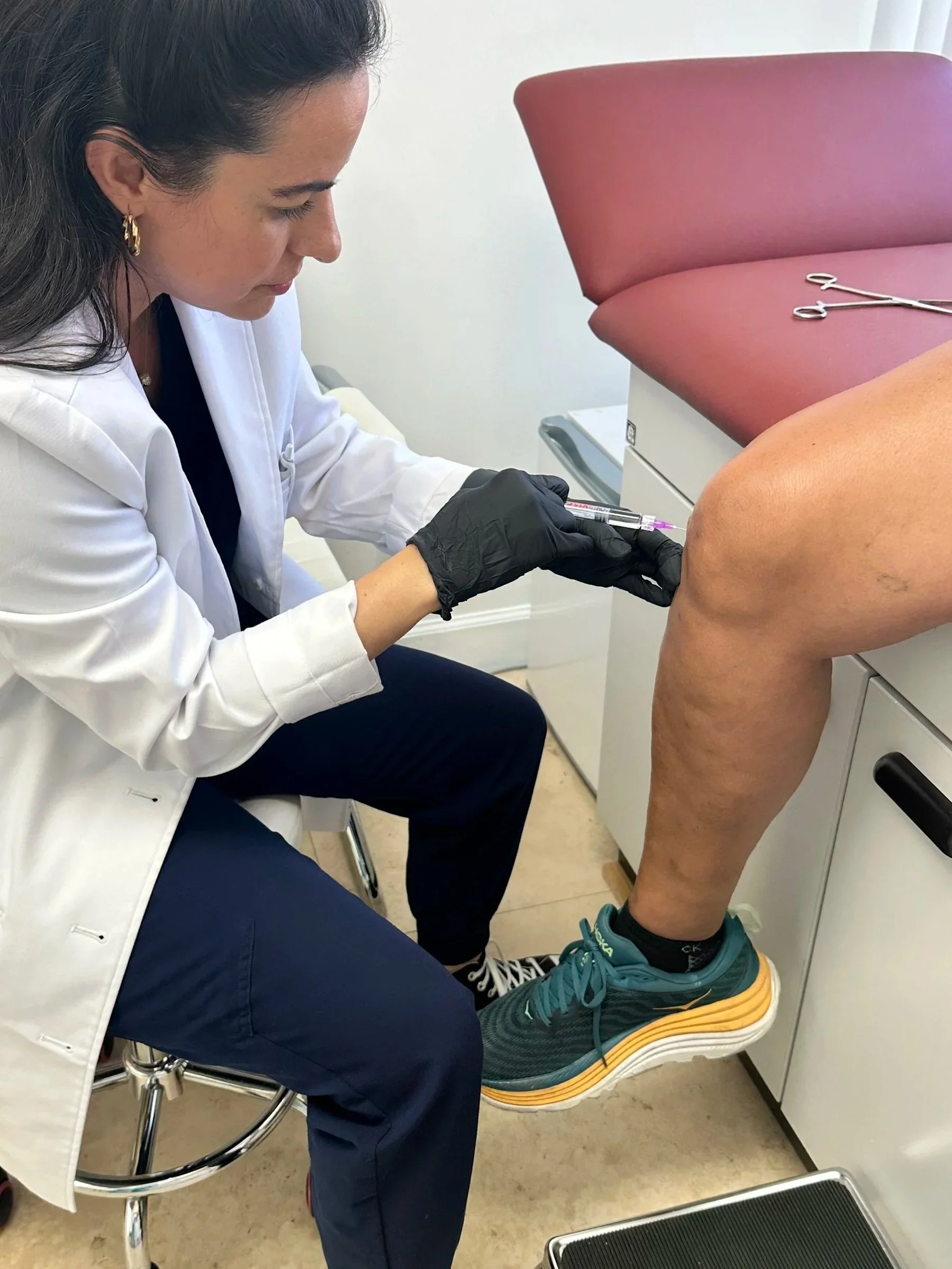
Joint Injections
Joint injections and joint aspirations may be done as part of a treatment plan for inflammatory joint conditions. Inflammatory joint conditions include rheumatoid arthritis, psoriatic arthritis, gout, tendinitis and bursitis, and osteoarthritis, among others.
What Is a Joint Injection?
A joint injection uses a needle to inject a medication directly into a joint, such as a knee. Medications commonly used by your Rheumatologist can include corticosteroids (sometimes called “cortisone or steroids”) and hyaluronic acid. Joint injections can decrease pain, inflammation, swelling, and stiffness, as well as improve overall mobility and activities of daily living. When medically necessary and properly done by a trained professional, joint injections can add benefit to the patient. Keep in mind that the positive effects of joint injections are not permanent. Improvements from a joint injection usually last a few months before wearing off. In some milder conditions, joint injections may produce longer periods of disease control, but this is by no means a guarantee.
Sometimes a joint has fluid (called joint effusion) and with the injection a joint aspiration is of greater benefit when performed together with the injection at the same time. This is achieved by using a needle to remove joint fluid, sometimes before a medication is injected into the joint. Removing joint fluid can provide pain relief and improve mobility. Fluid from a joint aspiration can be examined and sent for laboratory analysis. This helps us determine the cause of the joint effusion (joint swelling) and better help the patient with a more targeted therapy.

Hydroxychloroquine (Plaquenil)
Hydroxychloroquine (Plaquenil) is a type of medication in the category of disease-modifying anti-rheumatic drug (DMARD). It can decrease the pain/swelling from arthritis and prevent further joint damage. This medication is commonly used by your Rheumatologist to treat conditions such as Inflammatory arthritis, (Sle) systemic lupus erythematous, rheumatoid arthritis, Sjogren’s syndrome, diffuse systemic sclerosis, CREST syndrome, other connective tissue diseases, among others.
How To Take It
Hydroxychloroquine comes in an oral tablet you take as a daily pill. Adult dosing for rheumatic diseases ranges, typically, from 200 mg to 400 mg per day (typically 5 mg/kg, maximum 400 mg daily). It is usually taken as 2 divided doses daily every 12 hours. It is recommended to be taken with food to prevent gastrointestinal side effects. Symptoms can improve in one to two months, but it can take up to six months for the full benefits of this medication.
Before you start therapy you will need to have an eye exam by an Ophthalmologist (eye doctor) within the first year of use, then repeat every 1 year thereafter.
Regular laboratory monitoring is required while taking hydroxychloroquine every 3-6 months.
